Below are answers to a lot of questions you might have about Hypopressives- why not come along to a class and see what you think for yourself! www.hypopressivescotland.com
It is great to see a community of people who are dedicated to improving quality of life for women with pelvic floor issues learn about the Hypopresive Method. As you can imagine it is difficult to describe something in short blog posts, you tube videos when the skills and theory behind the method takes 60 hours to teach. It is also understandable that you should have doubts and questions as information in English is limited and the method is very unique.
Here are answers to some of your doubts.
This technique has been around since the 1980s so it isn’t new but it is just now making an entrance in the English speaking world. It is part of hospital procedures and postpartum recovery protocols in Belgium where it was first discovered and studied by Marcel Caufriez. Over 6000 therapists have been trained in the method and almost 2000 fit pros as well. Thankfully finally we have trainers in English speaking countries so you are finally hearing about the method. Since it has been used for years by uro-gyno physios to treat prolapses and incontinence it has a strong clinical backing.
We’re reviewing the English texts but do remember that the science concepts have been simplified for clients so most certainly they are incomplete for a professional. The neurophysiology concepts behind the method are very complex. Please see this blog for the 3 requirements for an exercise to be considered hypopresive: http://hypopresives.com/hypopresives/three-requirements
The neurophysiology concepts include hypopresives stimulating the pneumotaxic center (pontine) of the brain via hypopresive postures that are amplified by the apnea and ribflare causing hypoxia and hypercapnea. The neumotaxic center, which is responsible for the resting tone of the respiratory muscles (diaphragm, ab wall, pelvic floor, serratus anterior, etc.), responds via neurological divergence that stimulates an activation or decrease in tone in the various muscles. The neurophysiology concepts are far too complex to answer here. They are fully explored in the 60 hours of HM training our master trainers receive.
HM seeks to normalize the postural tone of the diaphragm and the results here are excellent. The concept is full unrestricted mobility of the diaphragm and to normalize its resting position. Not sure where you got the idea that HM “takes the descent of the diaphragm out of the picture”. Also the rib flare comes from the serratus anteriors which are the postural antagonists of the diaphragm and thus help relax the diaphragm. It isn’t the change in pressure that causes the involuntary contractions of the core when performing HM (it was the original hypothesis but it was proven incorrect via research as the contraction comes before the change in pressure when measured by a pressure gauge in the rectum/esophagus and deep EMG of the pelvic floor).
“Here’s the thing, we need that pressure gradient and fluctuation of pressure created by the diaphragm in the abdominal cavity for a host of functions: it triggers breath (take Mary Massery’s course everyone!), contributes to circulation of lymph and blood, massages organs and contributes to bowel movement, sets up rest/work cycles of our postural muscles, and contributes to postural control.”
Of course and that is why HM helps to normalize the diaphragm function. HM also improves vascularization and the latest studies are looking at lymp
h circulation which is also improved. HM also improves intestinal transit and it fantastic for correcting posture.
“So here are my questions: How do Hypopressives address these other functions of the global system that impact continence, digestion, circulation, respiration, postural stability, etc?”
HM is a global system that does just that. Via neurological divergencies muscle resting tone is improved which is the main reason for the improvements in continence, injury prevention, etc. HM stimulates the sympathetic nervous system which causes improvements in these areas as well. The rhythmic performance of the exercises works with the emotional system. Through the neurological divergencies muscle tone is normalized which aids in postural improvements, proper mobility, etc. The autoelongation used through the techniques normalizes curvatures of the spine (does not cause lumbar kyphosis like you commented) and allows for rehydration of the intravertibral disks. Respiratory parameters are improved via normalization of the tension in the upper airway muscles, improving the functionality of the diaphragm as well as changes on a cellular level such as improvements in hematocrit and EPO. Again, it is hard to summarize something that takes hours to explain during the courses.
“How does the person return to function when downward pressure from normalized breathing resumes (perhaps normalized breathing never does?) Or the downward displacement of impact loading occurs? “
HM reprograms the core to properly manage intra-abdominal pressures so daily function improves and risk of injury from prolapses is reduced. Removing excess postural tone from the diaphragm also is an important factor in optimal function. When people return to their previous activities (perhaps with impact) their bodies can handle these activities better with less risk.
“While Hypopressives is also trying to move us away from this extreme that caused so much abdominal pressure, have they done it with yet another extreme? Hypopressives feels to me like our over-focus on abs all these years….a willingness to sacrifice other parts of the system for the sake of one part.”
HM is a global system that takes into consideration not just the biomechanical parts but also the parasympathetic vs sympathetic nervous systems, the emotional system, the person’s diet, even the temperature of the room and color of the lights. It goes well beyond just abs and seeks to reprogram the person’s body map and balance out their nervous system as well as the musculoskeletal system.
“For example, in the video above you can see there is a huge use of neck muscles (Sternocleido-mastoids are very prominent) to pull this off.”
What you are seeing is yes, activation of the SCM but what makes it seem more prominent than it is is the decrease in thoracic pressure which creates indents at the collarbone.
“So they have improved prolapse (which really is awesome, don’t get me wrong) but now do they have headaches and jaw pain? For some that is worth the risk. And from an aesthetic point of view…are we trading unflattering bellies for barrel chests?”
Actually HM doesn’t cause headaches or jaw pain. Yes, some people in the beginning will have a hard time activating their serratus anteriors and will over use upper traps etc. But this shortly gets improved and the end result is less pain and activation of the proper muscles. HM doesn’t seem to create barrel chests. After the 30+ years of its use this hasn’t been noted.
“Where’d the organs go? Are they sure they are up?”
Organs are lifted up. It has been studied via ultrasounds and MRIs.
“And finally, yes, the pelvic floor needs to go up…but it still needs to learn to go down too, even if you have a prolapse or incontinence, and handle impact loading. How do Hypopressives address this need?”
HM seeks to improve resting tone of the pelvic floor and for it to have proper shock absorption abilities (including responding to pressure by moving down and back up). Marcel Caufriez has actually developed a “tonemeter” that measures the resting tone of the pelvic floor in addition to its ability to produce force.
“I did get a chance to “try” a basic Hypopressives activity at this years APTA Combined Sections Meeting. The session leader readily indicated this was her interpretation of the activity and I am readily admitting it was my attempt at interpreting that in my own body.”
It would be nice to know if the session leader had been trained by Marcel Caufriez or has just tried to understand the method via youtube… If she isn’t fully qualified to teach HM then she most likely wasn’t able to explain the method to everyone correctly.
“The result was I could feel my pelvic floor get sucked up involuntarily as I performed the maneuver. But it only stayed up as long as I held my breath and had my diaphragm in a locked position.”
HM has certain benefits that are very immediate and others that are achieved after the reprogramming phase is complete. Eventually the resting position of the internal pelvic organs changes but no, it does not happen after one day.
“What happens when things go back to “normal”? Or is breath holding their new norm? More questions”.
HM sessions usually last about 20 minutes during which people perform apneas and rest breaths. “Normal” breathing never ceases except during the apneas.
“Based on what I can decipher, Hypopressives appears to be another form of a static positioning and holds to achieve central stability. Another non-functional strategy when dynamic central stability is the goal.”
Your deciphering is a bit off track which is understandable due to the lack of information available to you. HM does just what you promote, improves dynamic central stability as it reprograms the core to do its job involuntarily.
I hope that has helped to answer some of these questions (and perhaps brought on some others). My initial reaction to this method was a bit like yours so I understand where you are coming from. I spent some years writing to associations in the USA for opinions and information (back in early 2000s) and none was available. So, please have some patience as it is a lot of work to get the information translated and available to the English speaking world. Plus the method is complex so the best way to learn is by doing the full courses and trying the techniques on yourselves and clients to see the fantastic results first hand. It is also important to note that we have thousands of colleagues around the world who are using these techniques with great success. That was what “won me over” in the beginning. I realized that pelvic floor physios wouldn’t continue to use a method that didn’t produce the desired results. Realizing that HM was the main rehab technique used for postpartum propelled me to learn more about it and trust that my colleagues were onto something that improved the quality of life for women.
Sunny greetings from Spain! Please let me know if I can be of further assistance.
Kaisa Tuominen
Hypopresive Method UK Country Master Trainer


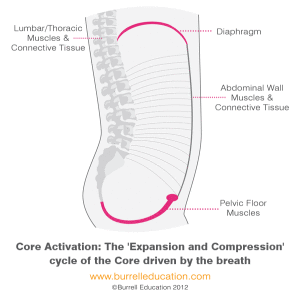 Many of us with our busy lives and the stress of money and the limited time we perceive that we have despite the technology that we now own that was supposed to allow us more time and freedom – which ultimately has tied us down more (but that’s for another rant at another time!!) – have forgotten how to breathe and use our rib cage and lungs properly.
Many of us with our busy lives and the stress of money and the limited time we perceive that we have despite the technology that we now own that was supposed to allow us more time and freedom – which ultimately has tied us down more (but that’s for another rant at another time!!) – have forgotten how to breathe and use our rib cage and lungs properly. If you look at the picture you can see that your rib cage is like the bellows that house your lungs – it follows that if you open and close your ribs you will allow more space for your lungs to inflate – you will also notice that your rib cage is not only at the front of your body!
If you look at the picture you can see that your rib cage is like the bellows that house your lungs – it follows that if you open and close your ribs you will allow more space for your lungs to inflate – you will also notice that your rib cage is not only at the front of your body!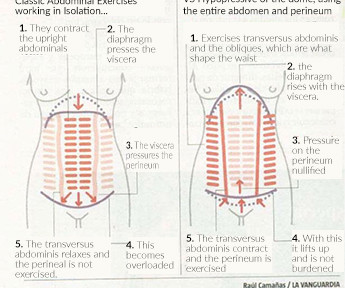
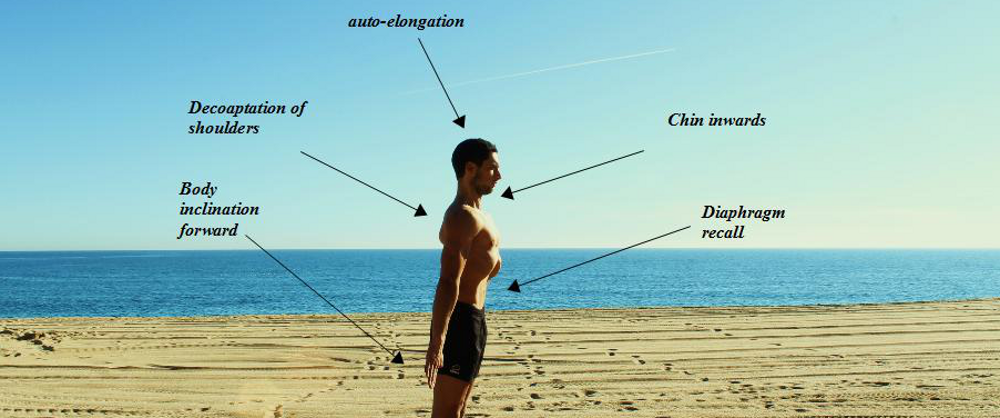











 Something for you to try first as doing and feeling is better than just reading.
Something for you to try first as doing and feeling is better than just reading.