Insights
Pathways to Pain Relief: Insights and Resources for Your Journey
What If Leaking Is a Threshold, Not a Failure?
If you leak when you run, jump, cough, sneeze, lift, walk downhill or rush to the toilet, it can feel frightening. But leaking does not always mean your pelvic floor is weak, damaged or failing. Sometimes it is your body showing you that your current strategy has reached its limit. In this blog, we explore how breath, posture, timing, fear, proprioception, surface choice, urgency and whole-body load sharing all influence pelvic floor symptoms.
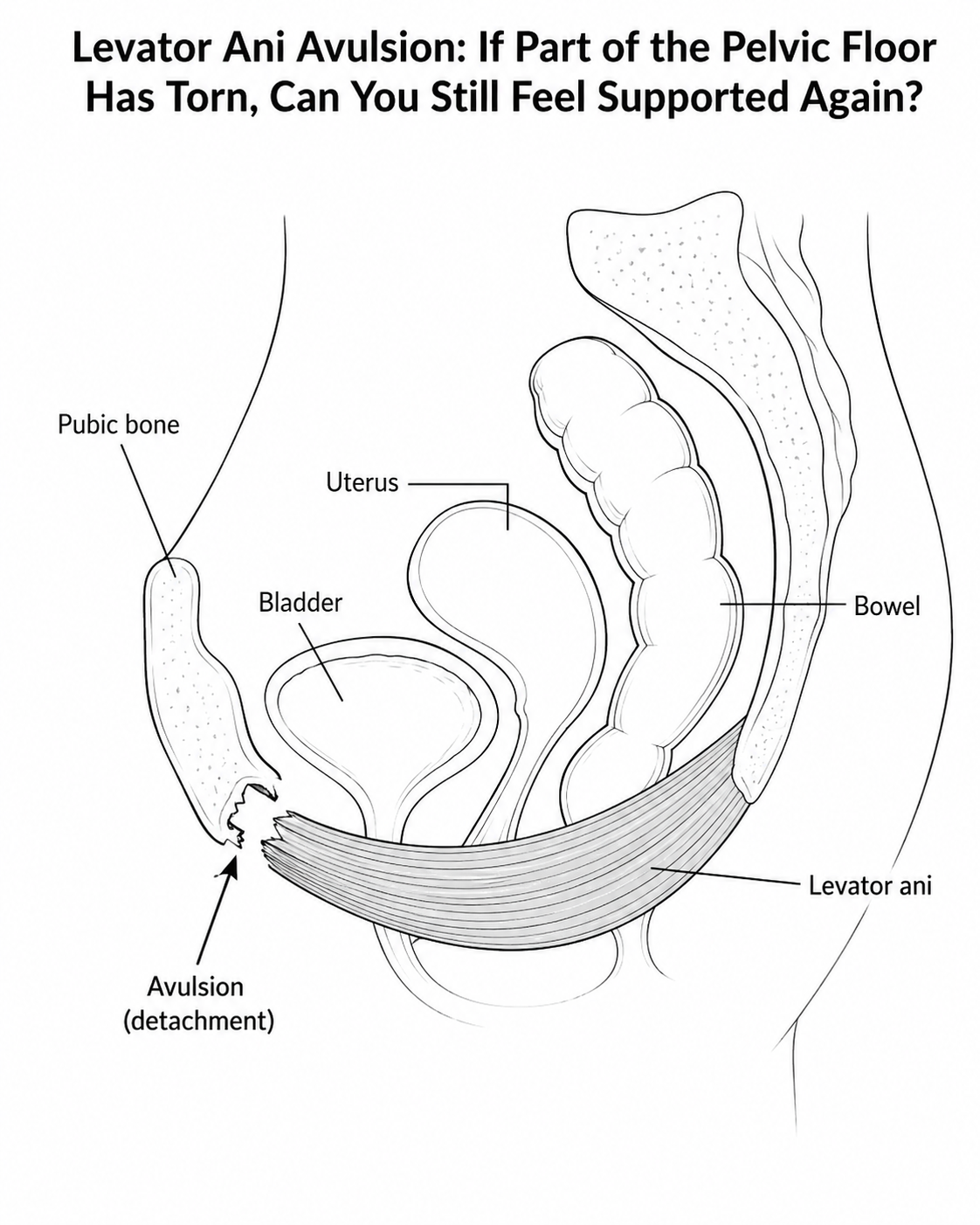
Levator Ani Avulsion: If Part of the Pelvic Floor Has Torn, Can You Still Feel Supported Again?
A levator ani avulsion means part of the deeper pelvic floor muscle has detached from its attachment point, often during childbirth. It can feel scary, especially if you have symptoms like heaviness, prolapse, leaking or a sense that your body no longer supports you in the same way. But torn does not mean hopeless. This blog explores what levator ani avulsion is, why support can still be rebuilt, and how breath, posture, pressure management and whole-body movement can help you feel more connected and confident again.
Women Are Seasonal: How Hormones Change the Way We Need to Move
Women’s bodies are not linear. From girlhood to menopause and wise womanhood, our hormones, nervous system, pelvic floor, muscles and recovery needs all change. This blog explores how movement can evolve through every season of a woman’s life, and why ageing does not mean doing less, it means learning to move with more awareness, strength and respect.
The Body Does Not Keep the Score, So Why Does the Body Still Matter?
A recent neuroscience paper challenges the idea that “the body keeps the score”, suggesting trauma may be less about storage and more about prediction. In this blog, Abby explores what that means for Hypopressives, TRE®, pelvic floor symptoms and the way we understand release, safety and healing through the body.
Women Are Not Small Men. But We Have Also Not become Suddenly Fragile Either.
Women are not small men, but we are not broken either. This blog explores why exercise after 40 needs a smarter conversation, one that includes hormones, pelvic floor health, breath, pressure, strength, fascia, recovery and the story your body has lived through.
Can Hypopressives Help with Prolapse?
Prolapse is not just about weakness. It is also about pressure, breath, posture and how the body responds to load. In this article, we look at what prolapse is, why symptoms happen, and how hypopressives may support bladder, uterine and bowel health as part of a gentle, non-surgical approach
Beyond Kegels: Why Your Postnatal Workout Plan Might Be Missing the Pelvic Floor
Many postnatal women are told to do Kegels, but still feel weak, leaky, or unsupported when they return to exercise. This blog explores why a postnatal workout plan needs more than squeezing, and how the Hypopressives Method can support reflexive strength, pressure management, and confident recovery after birth.
How to Relax Pelvic Floor Muscles Safely and Effectively
Why constant tightening can worsen pelvic pain, and how to restore balance through breath and decompression
For many women, the first piece of pelvic health advice they ever hear or find via internet searches is simple.
“Do your Kegels.”
The intention is good because strength really does matter, but strength alone is not the whole story.
In reality, many pelvic floor symptoms are not caused by weakness at all. They are actually caused by too much tension.
If the muscles of the pelvis are constantly bracing, gripping, or shortening, the system loses its ability to move freely. Pain, pressure and dysfunction can and often do follow.
Learning how to relax pelvic floor muscles is therefore not a sign of weakness. It is often the first step toward restoring healthy function.
Hypopressives Are Not Just Breathing: Why It’s Time to Rethink the “Internal Lift”
Hypopressives are often described as a vacuum or internal lift for the pelvic floor. But the method is far more intelligent than that. In this post, Abby explores the history of Hypopressives, why the old “lift” explanation is too simple, and how breath, pressure, fascia, posture, the nervous system and whole-body movement work together to support pelvic floor healing.
How the Bladder Really Works: Urgency, Leaks, Pelvic Floor and the Nervous System
Bladder symptoms are rarely just about the bladder. This blog explores how the kidneys, detrusor muscle, urethra, pelvic floor, brain, nerves, prolapse, scar tissue and stress all shape urgency, leaks and continence, with gentle practical ways to begin working with your body.
How to Keep Strengthening Your Pelvic Floor Once You Start Seeing Results
Seeing those first signs of progress can feel huge.
Maybe you are leaking less on walks. Maybe that dragging, heavy feeling has eased. Maybe your posture feels more open and your body more connected. These are not small wins. They are early signs that your system is starting to organise itself differently.
But this is also the point where many women quietly wonder, now what?
The truth is, pelvic health is not something we “fix” once and forget. It is something we build, maintain, and refine over time. The Hypopressives Method is not just a short rehab phase. It is a way of training your body to manage pressure more intelligently, organise posture more efficiently, and support pelvic floor strengthening as part of everyday life.
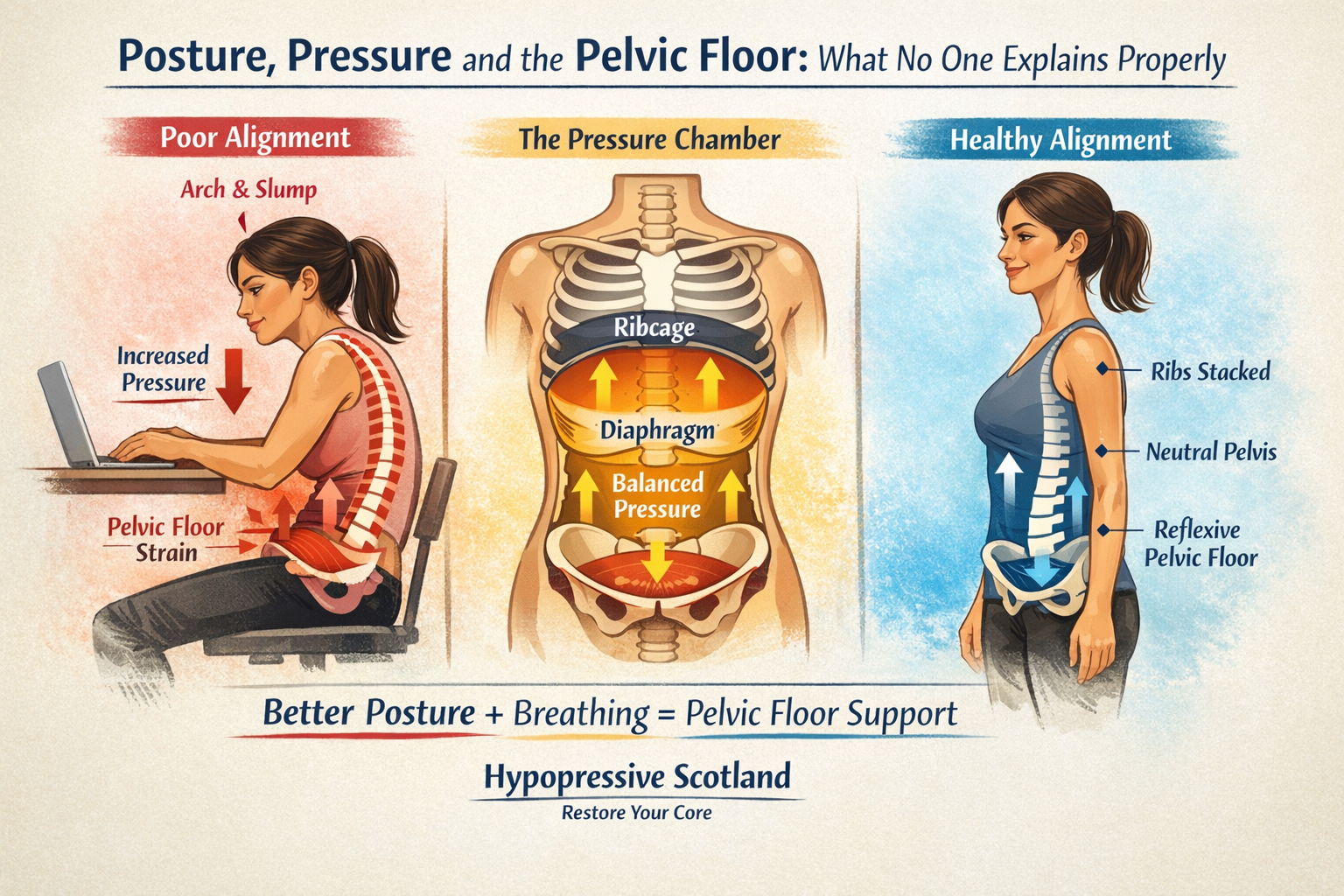
Posture, Pressure and the Pelvic Floor: What No One Explains Properly
Let’s clear something up straight away.
Posture isn’t all about looking taller, slimmer or more confident in your favourite wee black dress.
Posture is actually more about pressure. And when we talk about posture and pelvic floor health, what we are really talking about is how force moves through your body every single minute of the day.
Tiny Daily Movements for Pelvic Floor Support and Body Awareness
What if support did not only happen in a class or on a mat, but in the quiet little moments already woven through your day? This post explores how tiny daily movements can gently reshape breath, posture, pelvic floor support and the way you live in your body.
Beyond Kegels: Why Your Postnatal Workout Plan Might Be Missing the Pelvic Floor
Still doing your Kegels but not feeling the difference? This blog explores why postnatal recovery is about more than squeezing, and how the Hypopressives Method can help women restore reflexive strength, improve pressure management, and return to movement with more confidence.
The Silent Signs of Pelvic Floor Dysfunction Most Women Ignore
If you search for the signs of pelvic floor dysfunction, most articles will talk about leaking when you cough, sneeze, or run.
But pelvic floor problems very rarely begin there.
For many women, the early signs are quieter. They appear gradually in ways that are easy to dismiss. A strange heaviness at the end of the day. A feeling of pressure when standing for long periods. Lower back ache that appears for no obvious reason.
These symptoms are often labelled as common, particularly for women over 35 or after pregnancy.
But common does not mean normal.
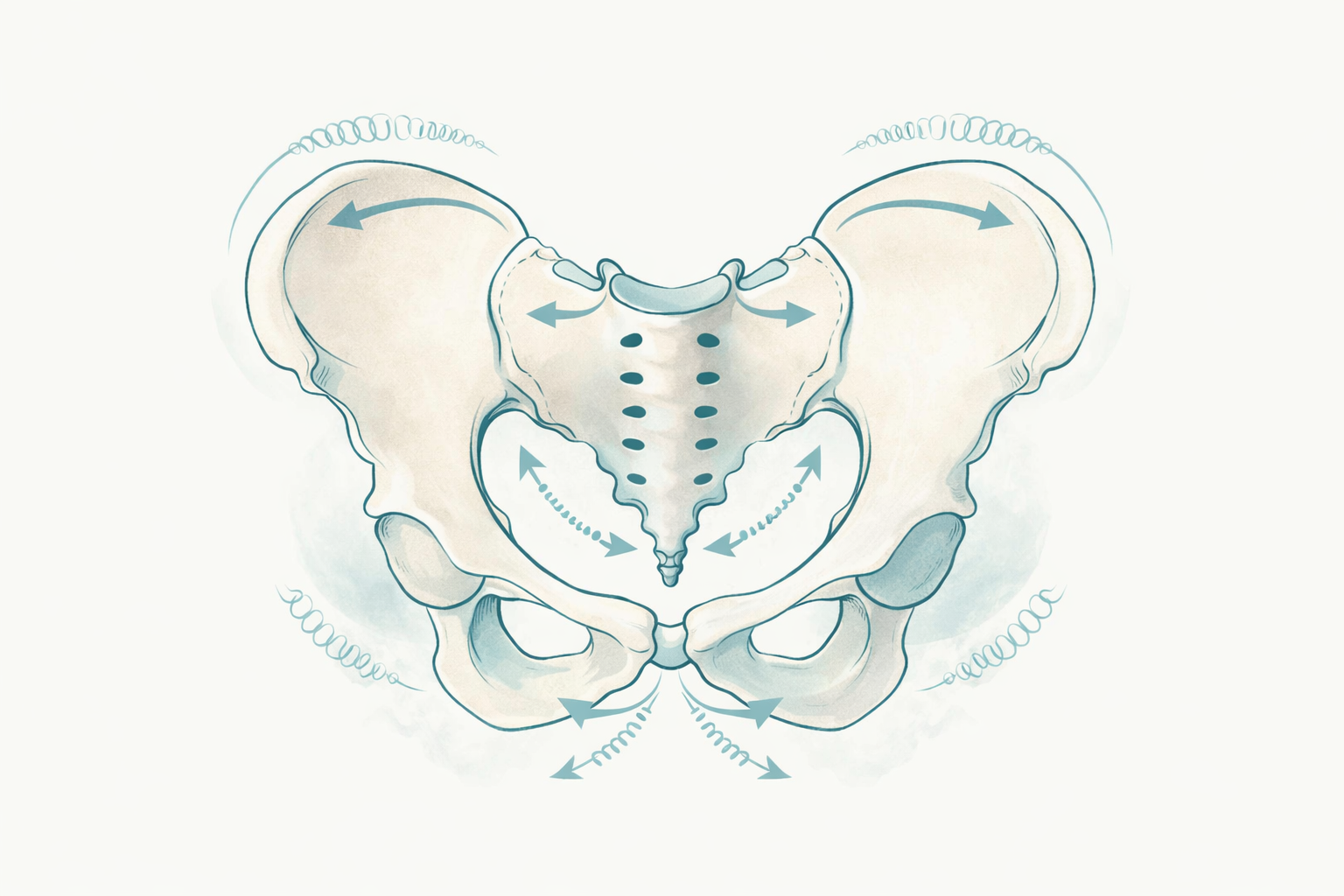
Why the ilia and sacrum need to move
The pelvis is absolutely not meant to be rigid. In this post, I explore why subtle movement between the ilia and sacrum matters for pelvic floor health, and how elasticity, viscoelasticity, fascia, breath, posture, and walking all shape the way the body manages force and pressure.
Trauma Release Exercises (TRE®️) for Pelvic Floor Tension: A Beginner’s Guide
If your pelvic floor feels tight, guarded, or unable to let go, more strengthening is not always the answer. This gentle guide explores how TRE® can help the body discharge stored tension, reconnect with safety, and work beautifully alongside the Hypopressives Method.
Signs Your Pelvic Floor Is Getting Stronger and Working Better
Pelvic floor recovery, as I have said in previous blogs that have touched on this topic, rarely arrives with fireworks.
There is no dramatic moment where everything suddenly feels fixed. No obvious muscle flex you can see in the mirror. No loud signal telling you that the work you have been doing is paying off.
The pelvic floor sits deep inside the body. It supports the bladder, uterus and bowel, works closely with the diaphragm and abdominal wall, and responds constantly to breathing, movement and pressure.
Because of this, progress is often subtle.
Many women only measure improvement by the absence of symptoms, no leaks, no heaviness, no discomfort. But pelvic floor recovery usually begins much earlier than that.
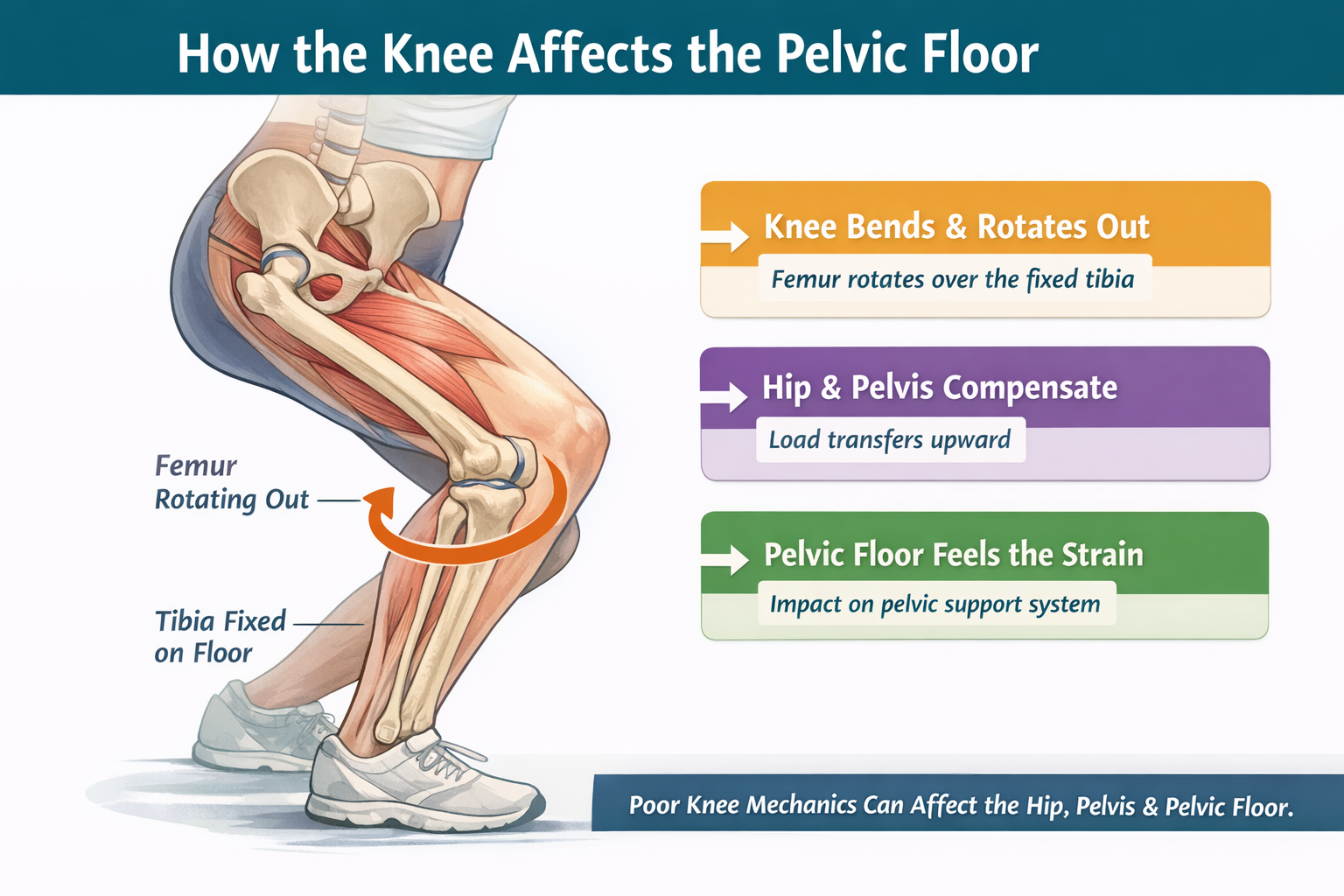
How Knee Mechanics Affect the Pelvic Floor | Hypopressive Scotland
The knee is not just a hinge. In this post, we explore how knee flexion, femur rotation, hip mechanics and pelvic organisation may all influence the pelvic floor. If symptoms show up in squats, stairs, walking or lunges, this whole-body connection matters.
Uterine Prolapse: Can You Actually Manage Symptoms at Home?
A diagnosis of prolapse can feel frightening and isolating, but many women with symptoms can improve comfort and confidence with conservative support. This blog explores uterine prolapse management at home, how pressure affects symptoms, and where the Hypopressives Method may fit within a learning to manage pressure, guided approach.